Trochanteric Bursitis
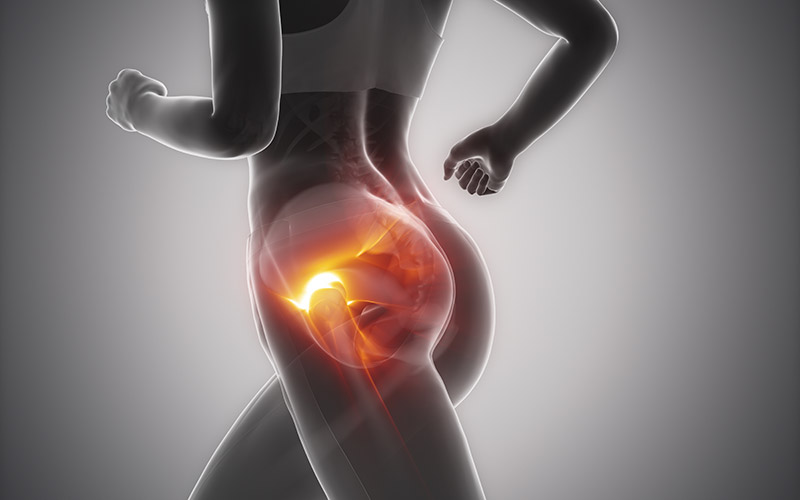
Hip pain is one of the more frequent complaints as people age, and many times it may be attributed to bursitis in the hip. Bursae are fluid-filled sacs that helps provide cushion between bone and soft tissue, and they can be found all over the body. When a bursa gets irritated or inflamed, it is referred to as bursitis. On the outside of the hip/upper thigh, there is a large bony point called the greater trochanter, and the trochanteric bursa is one of the more commonly affected areas where bursitis can occur (often referred to as trochanteric bursitis). Trochanteric bursitis can occur for a variety of reasons, including direct injury to the area, prior hip surgery, biomechanical factors like leg length differences or gait abnormalities, and overuse from repetitive activities like running, cycling, stair climbing, etc. Symptoms may include pain on the outer part of the hip that may or may not refer down the outside of the thigh or buttock, pain when lying on the affected side, pain getting in/out of the car or a deep chair, and pain with repetitive activities like walking, running, biking.
Conservative treatments like rest from overuse, ice, and NSAIDS may be effective to reduce inflammation and pain from trochanteric bursitis. Your doctor may also decide an injection may be beneficial to help relieve symptoms. Physical therapy can be very useful in helping reduce symptoms and prevent future exacerbations of pain as well. Exercises and manual interventions in physical therapy will aim to improve flexibility and mobility in surrounding areas that are tight, as well as improve strength in muscles that are weak, to improve the stabilization of the core, hips, and legs. Balance and proprioceptive exercises may also be given to help improve pelvic stability to aide with returning to your prior level of function.
If you have questions or would like more information on trochanteric bursitis, please contact us at ProActive Physical Therapy and Sports Medicine.
Reference:
Foran, Jared R.H. Hip Bursitis. https://orthoinfo.aaos.org . Reviewed September 2018. Accessed January 27, 2019.






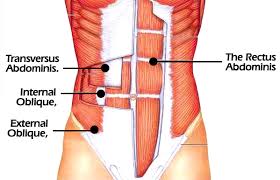 Whenever someone experiences pain in their low back, a phrase often heard is that they need a stronger “core.” The term “core” refers to several muscles primarily in the back/lumbar spine, abdominal region, and pelvis. When looking at the low back specifically, there is less bony stability than in the thoracic spine, which forces our muscles to provide the support needed to protect the low back. Two of the most important muscles in the core that provide this support are the transverse abdominis and the multifidus. These muscles act as a “back brace” (in addition to other core muscles) to help provide adequate spinal stability.
Whenever someone experiences pain in their low back, a phrase often heard is that they need a stronger “core.” The term “core” refers to several muscles primarily in the back/lumbar spine, abdominal region, and pelvis. When looking at the low back specifically, there is less bony stability than in the thoracic spine, which forces our muscles to provide the support needed to protect the low back. Two of the most important muscles in the core that provide this support are the transverse abdominis and the multifidus. These muscles act as a “back brace” (in addition to other core muscles) to help provide adequate spinal stability. Walking into a physical therapy evaluation can sometimes seem a little overwhelming if you do not know what to expect and have never completed therapy before. Although each therapist treats a little bit differently, here are some general guidelines that you can expect on your very first visit with a therapist at ProActive Physical Therapy.
Walking into a physical therapy evaluation can sometimes seem a little overwhelming if you do not know what to expect and have never completed therapy before. Although each therapist treats a little bit differently, here are some general guidelines that you can expect on your very first visit with a therapist at ProActive Physical Therapy.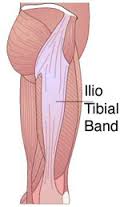 The IT-band (or iliotibial band) runs from the top of the pelvis, or ilium, and extends all the way down the outside of the thigh to the top of the lower leg, or tibia. In the thigh, it also connects to your glutes and tensor fascia latae muscles, and as it travels downward, has fibers that blend into your knee cap as well. The IT-band is made up of very dense connective tissue, making it extremely strong to provide stability during weight bearing activity. Functionally speaking, when we bend and straighten our knee repetitively (i.e. during running), the band slides back and forth and can sometimes cause localized irritation or inflammation. This can result in a very common sports related injury called IT-band syndrome. Symptoms can be felt anywhere along the IT-band, but usually occur closer to the attachment near the lateral knee. Muscle imbalances, like tight hip flexors or weak hip rotators, can often times be the cause of developing IT-band syndrome.
The IT-band (or iliotibial band) runs from the top of the pelvis, or ilium, and extends all the way down the outside of the thigh to the top of the lower leg, or tibia. In the thigh, it also connects to your glutes and tensor fascia latae muscles, and as it travels downward, has fibers that blend into your knee cap as well. The IT-band is made up of very dense connective tissue, making it extremely strong to provide stability during weight bearing activity. Functionally speaking, when we bend and straighten our knee repetitively (i.e. during running), the band slides back and forth and can sometimes cause localized irritation or inflammation. This can result in a very common sports related injury called IT-band syndrome. Symptoms can be felt anywhere along the IT-band, but usually occur closer to the attachment near the lateral knee. Muscle imbalances, like tight hip flexors or weak hip rotators, can often times be the cause of developing IT-band syndrome.